Abstract
Background. Although multiple myeloma (MM) has been known as an incurable disease for many decades, recent advances have extended the survival of MM patients, resulting in a cure among a significant proportion. Currently, it is not yet known which patients are able to survive long enough to consider the possibility of a cure. In order to identify patient subgroups that may have extremely favorable outcomes, an analytical approach that requires continuous and standardized follow-up is essential. Our dual-center database that dates to 2002 including 1554 newly diagnosed myeloma patients, is an ideal model for such an evaluation of trends in myeloma diagnostics and treatment outcomes.
Patients and Methods. We performed a retrospective dual-center analysis among newly diagnosed MM patients who were diagnosed before 2010 and had received autologous stem cell transplantation within our database of 1554 consecutive NDMM patients. 110 patients meeting these criteria were stratified by overall survival (OS): 0–5 years (Group 1, n=43), 5–10 years (Group 2, n=27), and 10–15 years (Group 3, n=40). Baseline characteristics, treatment strategies, depth of response, first progression-free survival (PFS-1), and available MRD data are compared. Maintenance treatment was not approved until 2018 in Turkiye post-ASCT patients.
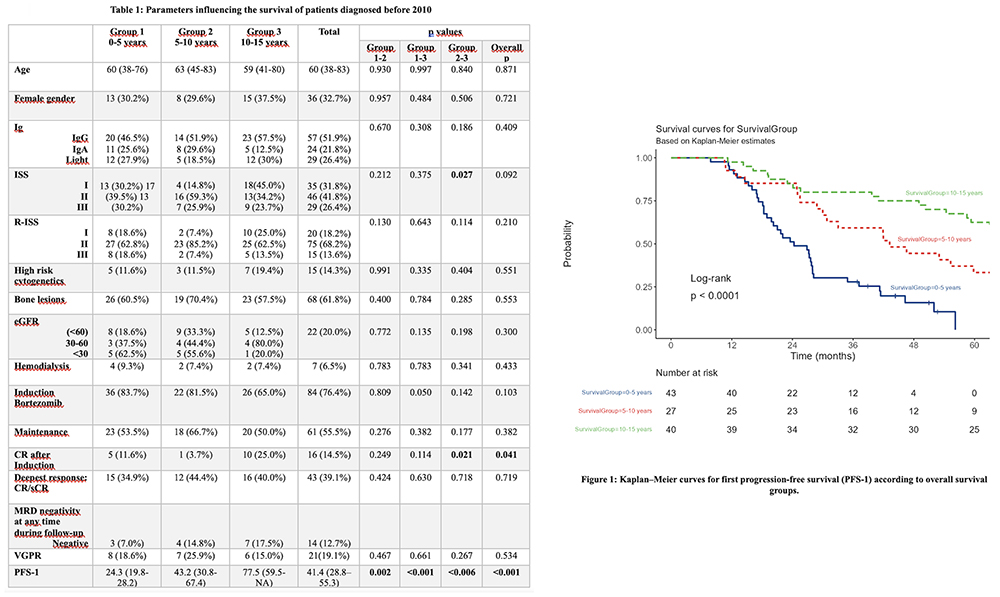
Results. Baseline disease characteristics, including R-ISS stage, high-risk cytogenetics but excluding ISS, and treatment protocols, were similar across survival groups. In contrast, outcome-related parameters clearly distinguished long-term survivors. The frequency of ISS-I was highest among 10–15-year survivors. Complete response after induction was significantly more frequent in Group 3 compared with Group 2 (25.0% vs 3.7%, p=0.021; overall p=0.041). As expected, median PFS-1 increased markedly across groups (24.3 vs 43.2 vs 77.5 months; overall p<0.001). MRD data were available for 37 patients, of whom 14 (37.8%) achieved MRD negativity at least once during follow-up. Among surviving patients with available MRD data (n=21), 10 (47.6%) achieved MRD negativity, and MRD negativity showed a non-significant trend toward enrichment among long-term survivors. Notably, a subset of patients achieved sustained remission off therapy, predominantly within Group 3.
Conclusions. These data provide compelling real-world evidence that a functional cure is not accidental but identifiable and achievable in MM. Long-term survival is primarily driven by ISS-I at diagnosis, both the depth and duration of first remission, pointing to the importance of drug sensitivity and an effective combination. Importantly, MRD negativity—although available in a limited subset—emerges as a biological hallmark of durable disease control and, together with sustained treatment-free remission, identifies approximately 9% of our patients in whom multiple myeloma may transition from a relapsing malignancy to a potentially curable condition.

Footnotes
Disclosures
No Conflict of interest.
Funding
No funding.
Article Information

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
