Abstract
Background. Bispecific antibodies (BsAbs) are an effective therapy for relapsed/refractory multiple myeloma (RRMM). Heterogeneity in depth and durability of response suggests host immune status is a key determinant. . Data on readily available immune biomarkers predicting response and resistance to BsAbs remain limited. This monocentric real-world study explores the impact of immune profiling and treatment sequencing on BsAb outcomes.
Methods. We prospectively analyzed RRMM patients treated with BsAbs at Hematology and Bone Marrow Transplantation Unit, Federico II University, Naples, Italy. Eligible patients had received ≥3 prior therapy lines and had measurable disease according to IMWG criteria. BsAbs included teclistamab, elranatamab, and talquetamab, administered per institutional protocols and regulatory indications. Peripheral blood samples were collected at predefined timepoints: baseline (prior to BsAb initiation), at 1 month after treatment start, after 4 months, and at disease progression or treatment discontinuation. Immune parameters included absolute lymphocyte count, CD8+ T-cell percentage by flow cytometry, and plasma IL-6 levels. When available, additional immunophenotyping was performed on peripheral blood and bone marrow aspirates. Patients were categorized by best IMWG response; responders achieved ≥VGPR, non-responders had stable or progressive disease. Sequencing variables included number of prior therapy lines and previous BCMA-targeted exposure. Correlations were assessed using Spearman’s rho; longitudinal changes were evaluated using Friedman test.
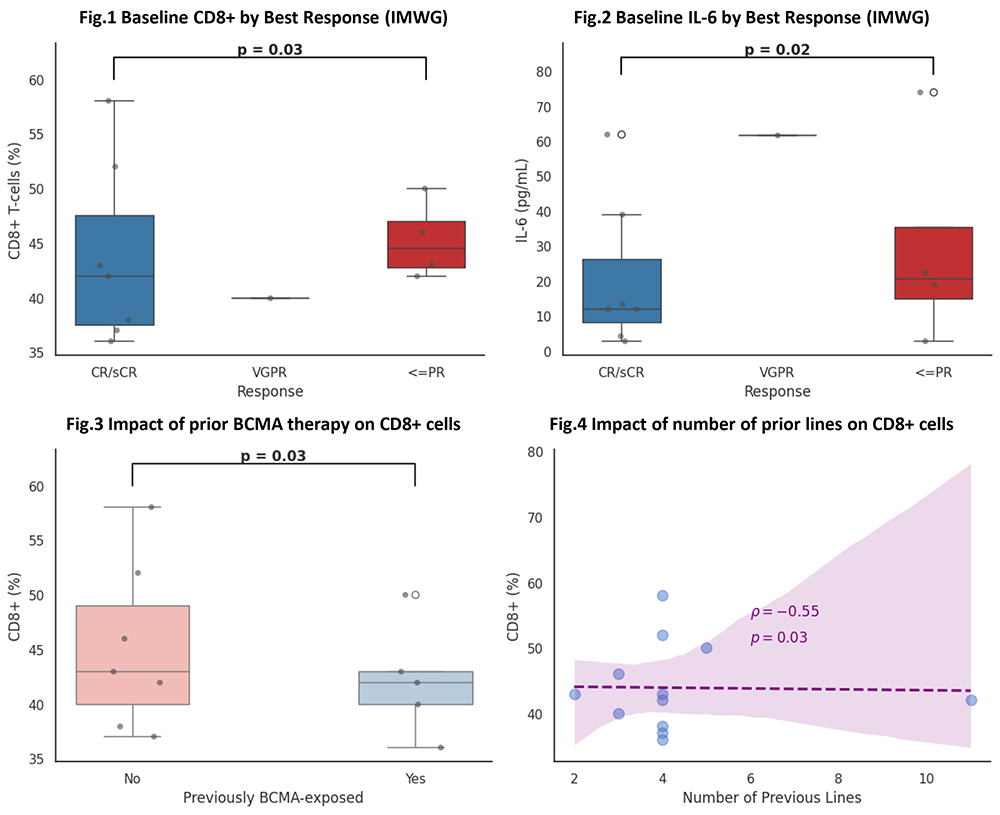
Results. Twelve patients were included (median age 74 years, range 54–80; 6 males), with a median of 4 prior therapy lines; 5 patients had prior BCMA-directed therapy. Eight patients received elranatamab and four teclistamab. Baseline CD8+ T-cell percentage differed significantly according to response: median 54% in CR/sCR, 45% in VGPR, and 38% in ≤PR (p=0.03, Figure 1). Baseline IL-6 levels were higher in inferior responders (median 12 pg/mL in CR/sCR vs 62 pg/mL in ≤PR; p=0.02, Figure 2). CD8+ inversely correlated with IL-6 (ρ=–0.62, p=0.01). Prior BCMA exposure and increasing number of previous therapy lines were associated with lower baseline CD8+ levels and reduced probability of deep response (ρ=–0.55, p=0.03; Figure 3-4). Patients with an “immune-favorable” profile (high CD8+, low IL-6) achieved CR/sCR even after multiple prior lines, whereas immune-unfavorable patients showed inferior outcomes. Longitudinally, responders maintained or increased CD8+ levels with declining IL-6 (Friedman p=0.04), while non-responders exhibited persistently low CD8+ and rising IL-6 (Friedman p=0.02).
Conclusions. Baseline immune profiling identifies distinct phenotypes associated with BsAb response in RRMM. An immune-favorable profile predicts superior outcomes even in heavily pretreated patients, while immune-unfavorable profiles may drive resistance. Prior BCMA exposure and treatment burden negatively impact immune fitness and response, underscoring the importance of sequencing. Despite the small monocentric cohort, the use of widely available biomarkers supports the development of an “immune asset score” to guide patient stratification and therapeutic decisions. Larger prospective studies are warranted.

Footnotes
Disclosures
No Conflict of interest.
Funding
No funding.
Article Information

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
