Abstract
Background. Interphase fluorescence in situ hybridization (iFISH) identifies recurrent chromosomal abnormalities in multiple myeloma (MM) that have strong and reproducible associations with progression-free and overall survival. International groups recognise specific iFISH abnormalities—del(17p), t(4;14), t(14;16), and 1q21 gain or amplification—as high-risk features that modify prognosis and increasingly influence treatment selection¹. Ireland has a stable and ageing MM population with improving survival, but variable availability of advanced diagnostics and novel therapies, as experienced in our cancer centre². This study provides real-world, population-specific insight into FISH-based MM biology in Irish patients.
Aims. To evaluate the frequency and prognostic impact of MM FISH abnormalities in our institution and compare findings with reported literature.
Methods. We retrospectively analysed clinical data from 69 patients with MM diagnosed and treated at our centre; FISH analysis was successful in 67 cases. Ethical approval was obtained and patient consent waived. Demographic data, disease subtype, IPI score, and FISH abnormalities were collected from electronic medical records and laboratory reports. IMWG prognostic criteria were used for FISH-based risk stratification, and genomic subgroups were examined for prognostic impact. Treatment regimens and responses were assessed using IMWG response criteria. Survival analyses were performed using Prism v10.06, with statistical significance defined as p<0.05 using the log-rank (Mantel–Cox) test.
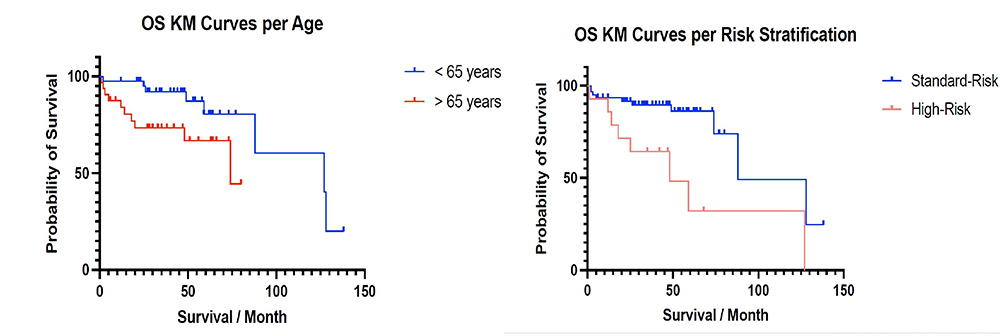
Results. Median age at diagnosis was 68 years, with a male predominance. IgG myeloma was the most common subtype (65%). Cytogenetic abnormalities were identified in 54% of patients, most frequently gain of 1q21 (33.3%). High-risk cytogenetics according to IMS 2025 criteria were present in 26.1% of patients. 10.8% harboured multiple high-risk lesions. A very good partial response or better was achieved in 72.5% of patients, and 37.7% underwent autologous stem cell transplantation. Median OS was significantly inferior in patients with high-risk versus standard-risk cytogenetics (48 vs 88 months, p=0.016) and in patients aged >65 years versus <65 years (74 vs 127 months, p=0.024). PFS and OS trends, and the frequency of high-risk FISH abnormalities, were comparable to published international data.
Conclusions. This study reports real-world outcomes of patients with MM treated at a regional Irish cancer center, focusing on the cytogenetic landscape and its prognostic significance. Demographic characteristics and the distribution of genetic abnormalities were comparable to large international series. High-risk cytogenetic features were associated with inferior survival outcomes, consistent with established prognostic models. These findings confirm that the biological behaviour and clinical impact of cytogenetic risk in MM are reproducible in an Irish population, supporting the generalizability of international risk stratification frameworks and reinforcing the importance of cytogenetic profiling in routine clinical practice.
References
1. Risk Rewritten: The Biology-Driven 2025 International Myeloma Society/International Myeloma Working Group Criteria for High-Risk Multiple Myeloma (2025) The Hematologist, 22(6), American Society of Hematology.
2. National Cancer Registry Ireland. Multiple myeloma (ICD-10 C90) cancer factsheet 2018–2020. Cork: NCRI; 2022.

Footnotes
Disclosures
No Conflict of interest.
Funding
No funding.
Article Information

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
