Abstract
Background. In patients with Multiple Myeloma (MM) chronic inflammation promotes malignant progression by altering tumor microenvironment and proliferation, with development of drug resistance. Aging itself is associated with a chronic low-grade inflammation, the so-called inflammaging, due to imbalance of the immune system. Interleukin-6 increases many inflammatory parameters, like Reactive C Protein (RCP), Fibrinogen (Fb) and Ferritin (Fe). However, the relationship between these inflammatory biomarkers and the prognosis of MM is still unknown.
Objectives. To provide an easy and cost-effective prognostic model, we evaluated inflammation parameters in newly diagnosed elderly (>75 years) patients with MM and correlated their levels with age, haemoglobin (Hb), ISS and overall survival (OS).
Methods. A cohort of 109 elderly patients with MM newly diagnosed in 11 hematology departments in central Italy from Jan 2019 to Apr 2025 was collected and analysed. Patients were stratified according to blood levels of RCP, Fb and Fe. An Inflammation score (I-score) was built by assigning 1 point each to elevated PCR, Fb and Fe and two different risk groups were defined: low-risk group (I-score 0) with 0-1 point and high-risk group (I-Score 1) with 2-3 points.
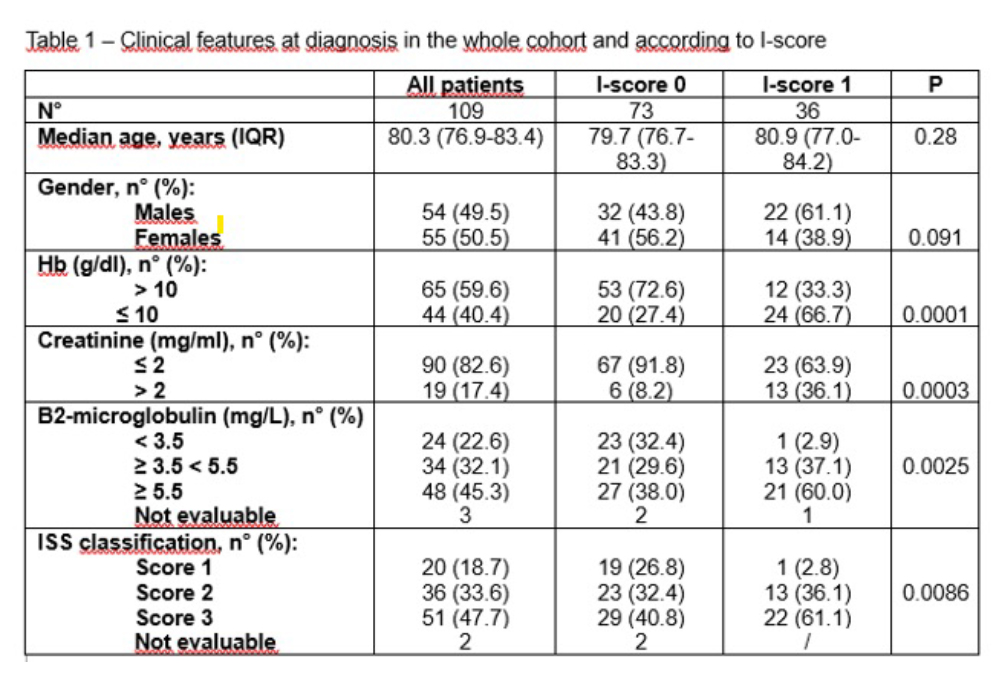
Results. Among the 109 patients, 73 (66.9%) had an I-score 0 and 36 (33.1%) an I-score 1. The main clinical features at diagnosis of the whole cohort and according to I-Score groups are reported in the Table: MM was preceded by MGUS and SM in 33,9% and 12,8% of the patients in the whole cohort, without differences between the two I-score groups. No difference was also observed between the two I-score groups as to median age (79.7 vs 80.9 years, p0.28). Patients in the I-score 1 had a significant higher rate of anemia (Hb ≤10 g/dl), renal impairment (creatinine levels > 2 mg/L) and β2 microglobulin elevation (p<0.0001, p 0.0003 and p 0.0025, respectively). In addition, the I-score 1 group had a higher rate of ISS 3 compared to the I-score 0 group (p=0.0086). As to treatment, 34 patients (31.19%) received dara-based triplets, 38 (34.8%) bortezomib-based doublets, 25 (22.9%) lenalidomide-based schemes and 12 (11%) MP and other low dose therapy. At the last follow-up, 67 patients (61,64%) are still alive, 5 (4,6%) were lost to follow-up and 36 (33%) died. Median OS of the whole cohort was 47.0 months (95%CI 32.0 – 65.0). Median OS of the I-score 0 group was 51.9 months (95%CI 38.3 – 72.3) compared to 30.2 months (95%CI 12.6 – 68.8) of I-score 1 group (p=0.0083).
Conclusions. I-score, which is very simple to assess, showed a good correlation with parameters of disease aggressiveness at diagnosis and with OS, implementing ISS staging and providing a cost-effective risk stratification tool. It could be a good method to identify high-risk MM patients, in particular among elderly patients, in which karyotypic and molecular analyses are not routinarily performed.

Footnotes
Disclosures
No Conflict of interest.
Funding
No funding.
Article Information

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
