Abstract
Introduction. Multiple Myeloma (MM) is a plasma cell dyscrasia characterized by the clonal proliferation of plasma cells, which is associated with a significantly increased risk of both thrombotic and hemorrhagic complications.
Aim. This ongoing prospective observational study aims to characterize platelet function and thrombin generation (TGA) in patients with newly diagnosed MM and to assess the impact of first-line therapy on these parameters.
Methods. To date, eighteen patients with newly diagnosed MM have been enrolled. Platelet function was evaluated using closure time (PFA200) and light transmission aggregometry (Born method) with four agonists: ADP (5 µM), Epinephrine (Epi) (10 µM), Collagen (Coll) (2 µg/mL), and Arachidonic Acid (AA) (1 mM). Thrombin generation (TGA) was assessed using the Calibrated Automated Thrombogram (CAT) assay. Baseline results were compared with historical healthy control cohorts. Intra-patient analysis was performed on 11 patients after four cycles of induction therapy (D-VTd or DRd). Statistical analysis was performed using R software (version 4.4). Comparisons between patients and controls were performed using the Wilcoxon rank-sum test and Pearson’s Chi-square test. For paired data the Wilcoxon signed-rank test was employed. Statistical significance was set at p < 0.05.
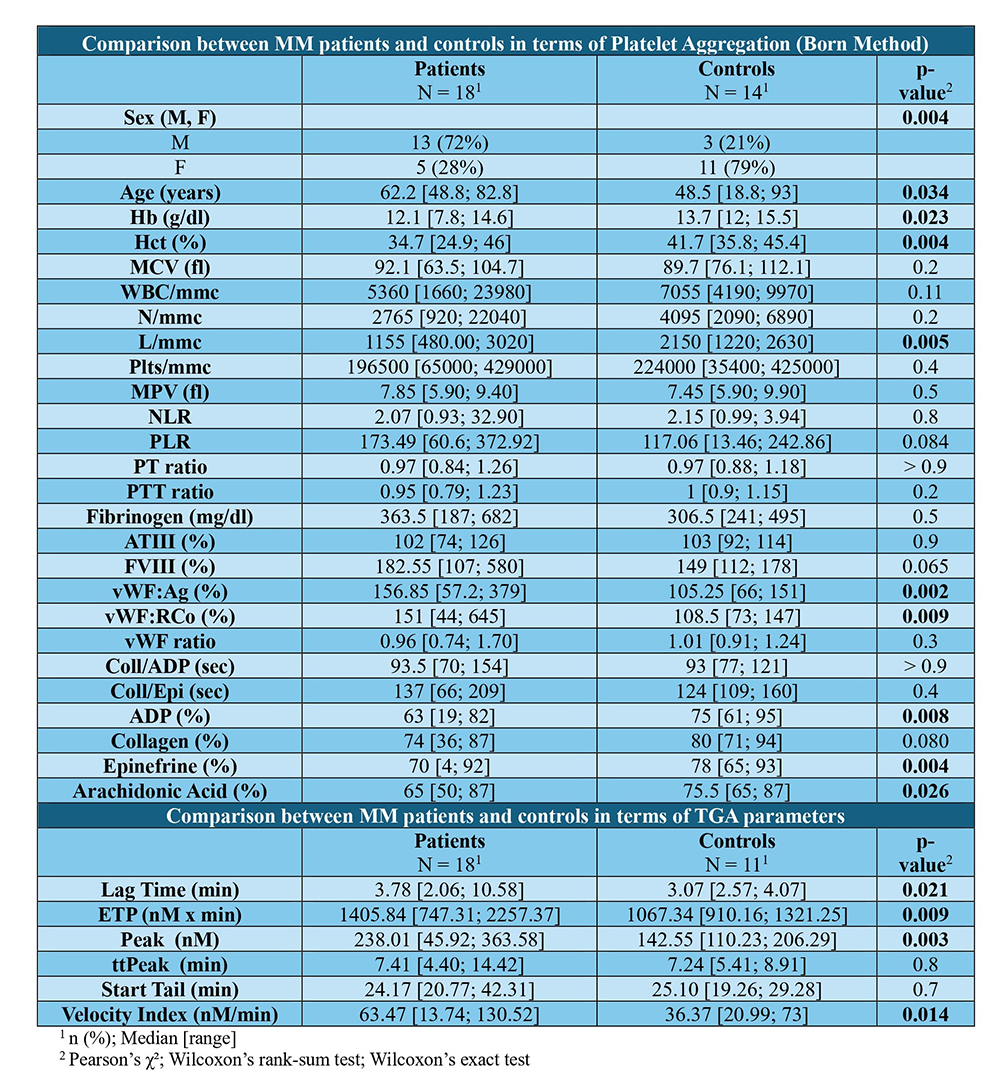
Results. In this interim analysis, at diagnosis, MM patients exhibited significantly lower platelet aggregation compared to controls for ADP (p=0.008), Epinephrine (p=0.004), and Arachidonic Acid (p=0.026). Procoagulant markers were significantly elevated: vWF:Ag (p=0.002) and vWF:RCo (p=0.009), while Factor VIII (p=0.065) showed a trend toward elevation. TGA analysis revealed significantly prolonged Lag Time (p=0.021) and significantly higher ETP (p=0.009), Peak (p=0.003), and Velocity Index (p=0.014) in MM patients (Table 1). Following therapy, most parameters remained stable, showing persistence of high thrombin generation, elevated vWF/FVIII levels, and impaired platelet function. Only Mean Platelet Volume (MPV) showed a significant decrease (7.85 fl vs. 7.30 fl, p=0.024).
Conclusions. This study highlights the coexistence of hypercoagulability and platelet dysfunction in MM. Based on these preliminary results, the reduction of tumor burden and the treatment don’t seem to modify the evaluated parameters.

Footnotes
Disclosures
No Conflict of interest.
Funding
No funding.
Article Information

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
